It seems to me that the number of patients is increasing, but the numbers of staff on the floor is the same. Coupled with sickness, annual leave and maternity leave it seems that the care is being put at potential compromise by this unbalanced position.
A&E's tend to have 3 areas, majors, minors and resus. They all need adequate nursing levels. It seems that time and time again that we are short. This means working harder than ever to provide the basics, not having breaks to their entirety (AND UNINTERUPTED) and morale and staff health plummeting. We are told we are over staffed, and the answer is long days. Hmmmm in the current environment E does not equal MC2. Staff will become more tired, stressed and mistakes will naturally occur. Check out the Dr's websites and DofH guidelines for proof.
But hey, I love the job. I thrive on the pressure, but I care about my patients and equally if not more about my friends and colleagues, and their well being.
However shit the department is, as labelled above, as long as there are limited breaches then the problem is not highlighted. Targets are good, but it needs to be taken in context of the whole health provision.
Sunday, 2 September 2007
Wednesday, 13 June 2007
Feeding our patients
The provision of nutrition to patients is an important part of nursing care. The provision of many aspects of services has been taken over by Carillion, a private company. As such there is difficulty in providing food to ED patients as it costs money. Wrong isnt it.
Saturday, 19 May 2007
Saturday, 5 May 2007
Dead dead dead
Patient from yesterday; died.
Ambulance service brought in a poorly patient. Refused conveyance from the first crew but later called them back. Brought in. Died. I saw the paramedic who went to him initially. I like this guy, he is compassionate, caring, intelligent and gives a shit. He is so cut up about this man who died, but he DECLINED to go to hospital. I tried to console this paramedic but he thinks he did wrong. He did NOTHING wrong.
Patients. The ones who are not sick want to go to hospital, the ones who are sick want to stay at home. Only God knows the time for our exit from this passage we call life.
Ambulance service brought in a poorly patient. Refused conveyance from the first crew but later called them back. Brought in. Died. I saw the paramedic who went to him initially. I like this guy, he is compassionate, caring, intelligent and gives a shit. He is so cut up about this man who died, but he DECLINED to go to hospital. I tried to console this paramedic but he thinks he did wrong. He did NOTHING wrong.
Patients. The ones who are not sick want to go to hospital, the ones who are sick want to stay at home. Only God knows the time for our exit from this passage we call life.
Friday, 4 May 2007
Goal Directed Therapy: An Urban Myth?
Goal directed therapy for sepsis. An ideal or an unachievable.
Middle aged man, recent urological surgery came to ED with confusion, hypotension and tachycardia. ABG showed a profound metabolic acidosis and WCC of 30. CRP also rather high at 340. Suggested aggressive intervention ie fluids, inotropes +/- vasopressors, central line and other intensive monitoring, such as a PA line. These were not carried out. A newly qualified, but savvy and competent staff nurse was the nurse dealing and was pushing tis but the drs were not going down this route.
The patiet was transferred down to CT. Next thing is the crash bleep announcing an arrest in the donut of death commonly known as CT. The man had crashed, purple plus major style. EMD arrest; chaos et al (except from my newly qualified colleague who was ace), widespread fluid from the man's stomach exacerbated the intubation, but control was achieved. EMD went to aystole and back to EMD. CPR continued and somewhat later an output was gained. Patient CT'd and then the drs argue about the deposition of the patient. For fucks sake, this is a 56 year old, this man needs ITU. he will probably die but he needs the oppotunity to attempt to live. ITU were not convinced, but common sense prevailed and we transferred the man to ITU. I don't hold out too much hope.
My main issue is that as a nurse who is relatively senior and experienced in emergency and critical care I feel so frustrated by the shackles that nursing entails when we have junior drs who have little experience of dealing with such ill patients. They don't take advice fom nurses and this grates me because I see patient care suffering. Goal directed therapy for whatever presentation sepsis, shock et al should be ALL our goals, but I fear that its not going to happen.
Middle aged man, recent urological surgery came to ED with confusion, hypotension and tachycardia. ABG showed a profound metabolic acidosis and WCC of 30. CRP also rather high at 340. Suggested aggressive intervention ie fluids, inotropes +/- vasopressors, central line and other intensive monitoring, such as a PA line. These were not carried out. A newly qualified, but savvy and competent staff nurse was the nurse dealing and was pushing tis but the drs were not going down this route.
The patiet was transferred down to CT. Next thing is the crash bleep announcing an arrest in the donut of death commonly known as CT. The man had crashed, purple plus major style. EMD arrest; chaos et al (except from my newly qualified colleague who was ace), widespread fluid from the man's stomach exacerbated the intubation, but control was achieved. EMD went to aystole and back to EMD. CPR continued and somewhat later an output was gained. Patient CT'd and then the drs argue about the deposition of the patient. For fucks sake, this is a 56 year old, this man needs ITU. he will probably die but he needs the oppotunity to attempt to live. ITU were not convinced, but common sense prevailed and we transferred the man to ITU. I don't hold out too much hope.
My main issue is that as a nurse who is relatively senior and experienced in emergency and critical care I feel so frustrated by the shackles that nursing entails when we have junior drs who have little experience of dealing with such ill patients. They don't take advice fom nurses and this grates me because I see patient care suffering. Goal directed therapy for whatever presentation sepsis, shock et al should be ALL our goals, but I fear that its not going to happen.
Friday, 27 April 2007
Getting Home
Why is it that patients become unable to get home once discharged. They automatically assume the God-given right to free transport home; either a paid taxi, or worse a frontline 999 ambulance. I can have a certain understanding of the little old chap or lady being taken back to their residential home, but grown adults of 18 plus.
Oh but I pay taxes they sqwark, well no shit, so do I. Find your own way home, you should'nt have been here in the first place.
The drunks are the best; what would you have done if you hadn't fallen over and twatted yourself on the head? you ask. Oh, I would have had a taxi or pulled. Right then dickhead, go and find one now.
Gomer.
Oh but I pay taxes they sqwark, well no shit, so do I. Find your own way home, you should'nt have been here in the first place.
The drunks are the best; what would you have done if you hadn't fallen over and twatted yourself on the head? you ask. Oh, I would have had a taxi or pulled. Right then dickhead, go and find one now.
Gomer.
Monday, 19 March 2007
Take Away?!?
Had a 86 year old post arrest. Flat and not particularly healthy. Shocked a couple of times by the paramedics and once by myself. A rather pro-active medical registrar suggested thrombylisis which was duly given, however the proglonged event lead to a termination of actively treating her.
Then the problems arose. The first two members of the family refused to believe she was going to die, and would not allow extubation til their sister arrived. Fine we said expecting them to be local. But hey no, they were coming from Wales. Didn't they know about breaches. Needless to say I had to try and keep this lady alive til these family members arrived. Cue ventilator and a bit of luck.
The family eventually arrived, and were with Mum. I extubated and 5 minutes later she died, with her family present. It gave the family some comfort.
As I was leaving one of the daughters came up to me and said that they wanted to take mum 'home with them'. Small problem she was dead.
Unfortunately not I said, as she was now the property of the coroner and it would be theft, also unethical and unhygenic. The transportation issue would have been fun too. A longboard and roof rack were mentioned.
Relatives are bizarre.
Then the problems arose. The first two members of the family refused to believe she was going to die, and would not allow extubation til their sister arrived. Fine we said expecting them to be local. But hey no, they were coming from Wales. Didn't they know about breaches. Needless to say I had to try and keep this lady alive til these family members arrived. Cue ventilator and a bit of luck.
The family eventually arrived, and were with Mum. I extubated and 5 minutes later she died, with her family present. It gave the family some comfort.
As I was leaving one of the daughters came up to me and said that they wanted to take mum 'home with them'. Small problem she was dead.
Unfortunately not I said, as she was now the property of the coroner and it would be theft, also unethical and unhygenic. The transportation issue would have been fun too. A longboard and roof rack were mentioned.
Relatives are bizarre.
Sunday, 4 March 2007
The wheat from the chaff
The Trust is desperately trying to reach the Government target of 98% of patients are dealt with within 4 hours. |For the most part we have been doing well; that was until Friday. Two breaches by lunch and more than twenty by the end of the day.
I came across a senior sister crying as she was doing her best. Is it a good working environment when people, granted even the least clinically credible sister (although a decent person) is reduced to tears by virtue of the atmosphere. Maybe they are trying to cull those who cannot control the department, but when there are no beds available breaches will occur. And when there are sick patients, which they have been and there are shortfalls in nursing staffing levels then this will become the norm for breaches to occur.
On top of that we have been awarded a 1.5% pay rise this year by Patricia (No clue) Hewitt, lee than the rate of inflation. What an insult to the hard work by nurses up and down the country! Get a grip, the Medical training is ballsed up, the waiting lists are manipulated with minimum waiting times, MRSA is rife and nurses are becoming scapegoats, the NHS needs to be revolutionised by those who understand it; the NHS staff, not idiots in the DofH.
I came across a senior sister crying as she was doing her best. Is it a good working environment when people, granted even the least clinically credible sister (although a decent person) is reduced to tears by virtue of the atmosphere. Maybe they are trying to cull those who cannot control the department, but when there are no beds available breaches will occur. And when there are sick patients, which they have been and there are shortfalls in nursing staffing levels then this will become the norm for breaches to occur.
On top of that we have been awarded a 1.5% pay rise this year by Patricia (No clue) Hewitt, lee than the rate of inflation. What an insult to the hard work by nurses up and down the country! Get a grip, the Medical training is ballsed up, the waiting lists are manipulated with minimum waiting times, MRSA is rife and nurses are becoming scapegoats, the NHS needs to be revolutionised by those who understand it; the NHS staff, not idiots in the DofH.
Friday, 2 March 2007
Trauma Continued
This is from the respected Trauma.org website on the management of severe Head Injuries.
(Us ED folk DO know what we are talking about) (most of the time).
Assessment of brain injury hinges on evaluation of the Glasgow Coma Score (GCS) and examination of the pupils. Traditionally a GCS of below 9 is considered to reflect severe brain injury. However with improvements in prehospital care and greater knowledge of brain injury, patients are arriving in emergency departments earlier and their brain injury may still be evolving. Therefore the following measures should be considered and porbably instituted in all patients with coma scores of 12 or below.
Management
The specific goals in the acute management of severe traumatic brain injury are:
1. Protect the airway & oxygenate
2. Ventilate to normocapnia
3. Correct hypovolaemia and hypotension
4. CT Scan when appropriate
5. Neurosurgery if indicated
6. Intensive Care for further monitoring and management
Hypoxia and hypotension are the greatest threat to functional outcome in brain injury. Early acute control of the above three parameters may have more impact than all other measures subsequently employed. Progressive neuronal loss occurs from the time of injury, not the time of arrival in hospital. Rapid sequence intubation should be used where available to secure the airway and maximally oxygenate the patient. Hypovolaemia and hypotension must be corrected early and take priority over other interventions for the brain injury. Other injuries causing haemorrhage must be addressed first (or simultaneously) so that an adequate cerebral perfusion pressure is maintained. Patients should be kept sedated to prevent coughing or valsalva maneuvers from fighting the ventilator, as these increase intracranial pressure.
(Us ED folk DO know what we are talking about) (most of the time).
Assessment of brain injury hinges on evaluation of the Glasgow Coma Score (GCS) and examination of the pupils. Traditionally a GCS of below 9 is considered to reflect severe brain injury. However with improvements in prehospital care and greater knowledge of brain injury, patients are arriving in emergency departments earlier and their brain injury may still be evolving. Therefore the following measures should be considered and porbably instituted in all patients with coma scores of 12 or below.
Management
The specific goals in the acute management of severe traumatic brain injury are:
1. Protect the airway & oxygenate
2. Ventilate to normocapnia
3. Correct hypovolaemia and hypotension
4. CT Scan when appropriate
5. Neurosurgery if indicated
6. Intensive Care for further monitoring and management
Hypoxia and hypotension are the greatest threat to functional outcome in brain injury. Early acute control of the above three parameters may have more impact than all other measures subsequently employed. Progressive neuronal loss occurs from the time of injury, not the time of arrival in hospital. Rapid sequence intubation should be used where available to secure the airway and maximally oxygenate the patient. Hypovolaemia and hypotension must be corrected early and take priority over other interventions for the brain injury. Other injuries causing haemorrhage must be addressed first (or simultaneously) so that an adequate cerebral perfusion pressure is maintained. Patients should be kept sedated to prevent coughing or valsalva maneuvers from fighting the ventilator, as these increase intracranial pressure.
Another Life Saved!!!!
Yet again our Trust, or more correctly ITU surpasses its self in its ability to F*%K up trauma care management. Well, rephrase that, certain itu members have the innate ability to bugger up the patients process.
Trauma shout, man verses bus. Exceptionally agitated with head, facial and chest injuries. Typical pre-alert, just agitated male. It took 7 people to hold down this ten stone man, who did not have english as his first language. I think he was saying 'I need a tube', but hey the gasman wasn't listening. The team leader; ED Physician states this man needs RSI and a tube, our Consultant stated this man needed a tube, even I stated that he needed a tube. (Incidently his shattered mandible was causing an interesting gurgling to emit from this patient). Seconds led to minutes, and after 15 minutes the ITU SHO said he needed to check with his consultant before tubing!!!!!! (who was not in resus). Hmmm thats a new ATLS guideline is it. He would have no hesitation tubing a 95 yr old purple plus, but baulked at this. Idiot.
Eventually he was tubed and ventilated.
Injuries as follows:
Mandibular # (in 3 places),
CT NAD (wait for the difuse axonal injury to develop....),
R Pneumothorax,
R Acetabular # (comminuted).
Significant traumatic injuries.
The Pneumothorax was going to be managed conservatively, but he is receiving IPPV therefore an indication for urgent chest drainage. This had to be pushed to be done, and then it was placed sub cutaneously.
The decision then was to extubate and place on a ward. I argued so stongly to get him on HDU, but our Trust has amalgamated ICU and HDU, and it is nigh on impossible to get onto the unit. Post extubation he gurgled for 10 minutes requiring suction, a joke.
This man went to a surgical ward (no monitor etc), and fortunately was still alive the next day. It is so frustrating that the people who manage trauma effectively, i.e. us the ED staff are run roughshod over by clinicians who have no comprehension of polytrauma and its effects. ATLS guidelines, textbooks, even Blue Peter give definitive guidance on Trauma Management. Can there be any clinical justification in these clinicians management and 'ownership' of the ET tubes. No there cannot, I trust to God that there won't be an incident when someone will die by virtue of this route. I and my more clued on colleagues cannot be available all the time, if only the book is followed!!!
Needless to say I suffered major trauma to my foot as I kicked the wall in frustration. Not a good shift.
Trauma shout, man verses bus. Exceptionally agitated with head, facial and chest injuries. Typical pre-alert, just agitated male. It took 7 people to hold down this ten stone man, who did not have english as his first language. I think he was saying 'I need a tube', but hey the gasman wasn't listening. The team leader; ED Physician states this man needs RSI and a tube, our Consultant stated this man needed a tube, even I stated that he needed a tube. (Incidently his shattered mandible was causing an interesting gurgling to emit from this patient). Seconds led to minutes, and after 15 minutes the ITU SHO said he needed to check with his consultant before tubing!!!!!! (who was not in resus). Hmmm thats a new ATLS guideline is it. He would have no hesitation tubing a 95 yr old purple plus, but baulked at this. Idiot.
Eventually he was tubed and ventilated.
Injuries as follows:
Mandibular # (in 3 places),
CT NAD (wait for the difuse axonal injury to develop....),
R Pneumothorax,
R Acetabular # (comminuted).
Significant traumatic injuries.
The Pneumothorax was going to be managed conservatively, but he is receiving IPPV therefore an indication for urgent chest drainage. This had to be pushed to be done, and then it was placed sub cutaneously.
The decision then was to extubate and place on a ward. I argued so stongly to get him on HDU, but our Trust has amalgamated ICU and HDU, and it is nigh on impossible to get onto the unit. Post extubation he gurgled for 10 minutes requiring suction, a joke.
This man went to a surgical ward (no monitor etc), and fortunately was still alive the next day. It is so frustrating that the people who manage trauma effectively, i.e. us the ED staff are run roughshod over by clinicians who have no comprehension of polytrauma and its effects. ATLS guidelines, textbooks, even Blue Peter give definitive guidance on Trauma Management. Can there be any clinical justification in these clinicians management and 'ownership' of the ET tubes. No there cannot, I trust to God that there won't be an incident when someone will die by virtue of this route. I and my more clued on colleagues cannot be available all the time, if only the book is followed!!!
Needless to say I suffered major trauma to my foot as I kicked the wall in frustration. Not a good shift.
Thursday, 8 February 2007
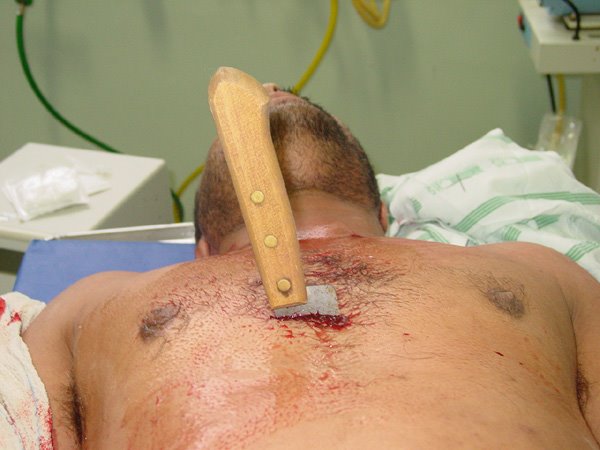
Stab Victim
Had a bloke brought in feeling sorry for himself. Been stabbed in the back and had a laceration to his scalp. Was attacked by a mad man he said. Met him at the ambulance door and in the 20 seconds it took from being off loasded from the ambulance to coming into A&E he had managed to smoke a rolly.
By the time I left I wanted to stab him too, annoying GOMER!!!!
By the time I left I wanted to stab him too, annoying GOMER!!!!
Saturday, 3 February 2007
Time of the month!!!!
Had a spotty chav and his chavette girlfriend attend A&E. He rushed in like it was an emergency.
'Have you got any paracetamol?' piped up the boy chav; 'she's got period pains'.
'Nope' we all replied. They left. Obviously confused themselves thinking we gave a damn!
GOMERS!!!!
'Have you got any paracetamol?' piped up the boy chav; 'she's got period pains'.
'Nope' we all replied. They left. Obviously confused themselves thinking we gave a damn!
GOMERS!!!!
Donor Cycle
At last, a trauma worth shouting about. Motorcyclist verses concrete bollard at high speed.
ABC's were deranged, he had a GCS of 3 and multiple pelvic and bilateral femur fractures. He was fortunately intubated quickly as things were not looking grand.
It was them the delays occurred.
A long wait for CT, a long wait in CT and then a long wait to ITU. Not straight to theatres. Fortunately the patient did not breach. (Joke). Not a good prognosis as he was developing coagulopathy and profound metabolic acidosis
It frustrates me intensely that patients wait so long to reach their appropriate destinations. Early intervention in trauma leads to potentially better outcomes. All the hard work initially carried out can be so easily let down when the patient reaches coagulopathy and then becomes unfit for surgery.
Who's heads do I bang together?
ABC's were deranged, he had a GCS of 3 and multiple pelvic and bilateral femur fractures. He was fortunately intubated quickly as things were not looking grand.
It was them the delays occurred.
A long wait for CT, a long wait in CT and then a long wait to ITU. Not straight to theatres. Fortunately the patient did not breach. (Joke). Not a good prognosis as he was developing coagulopathy and profound metabolic acidosis
It frustrates me intensely that patients wait so long to reach their appropriate destinations. Early intervention in trauma leads to potentially better outcomes. All the hard work initially carried out can be so easily let down when the patient reaches coagulopathy and then becomes unfit for surgery.
Who's heads do I bang together?
Tuesday, 30 January 2007
Breaches before safety!!
Some wag (not me) changed a screen saver on the works pc to: 'A&E Breeches before safety'. Just about sums up the culture at present.
Had a patient who became unwell just prior to transfer. 10 minutes before her 4 hour time was up. Vitals were ok, repeat ecg not too bad, but the sister in charge was almost losing it trying to move this patient out before she breached. This was the same sister who earlier tried to place a highly clinically unstable patient with a PE into a low dependency bed on the clinical decisions unit. One look at this patient tells you they are sick, however add that to her poor vital signs leads to the fact this person needs a higher dependency bed. I made sure she got one, and was castigated by this sister for doing this.
Therefore, the wag who typed 'breaches before saftey' is right on the ball when it comes to summing up the current climate in my A&E Deopartment. It is not helped when some of our seniors lack clinical acumen.
Had a patient who became unwell just prior to transfer. 10 minutes before her 4 hour time was up. Vitals were ok, repeat ecg not too bad, but the sister in charge was almost losing it trying to move this patient out before she breached. This was the same sister who earlier tried to place a highly clinically unstable patient with a PE into a low dependency bed on the clinical decisions unit. One look at this patient tells you they are sick, however add that to her poor vital signs leads to the fact this person needs a higher dependency bed. I made sure she got one, and was castigated by this sister for doing this.
Therefore, the wag who typed 'breaches before saftey' is right on the ball when it comes to summing up the current climate in my A&E Deopartment. It is not helped when some of our seniors lack clinical acumen.
Saturday, 27 January 2007
Cheating Death Part I
As an A&E Nurse it seems I get more dead people than the local Co-Op Funeral Shop. It comes with the territory that I get people die.
The other day I had 4 cardiac arrests! 3 died and one I dispatched to the ward. 25% success, not bad for a failing trust. Cheating death is always a losing battle but I will give it my best shot. The only downside is the relatives. I have lost count of the times that I have had to tell a relative that their loved one has shuffled unwillingly off this mortal coil. It can be heartbreaking. I have not become immune to this suffering, it affects me, however I can often be strong to the point of brutal dispassion. I can often be weak as well.
The young drug addict who dies, the RTA who was drunk and crashed into a tree. These deaths although sad are emotionally reconcilable. The 32 year old cardiac arrest who just drops is just shit though. Most of the time in A&E and in the NHS it is just a case of processing patients. A bit like Tesco's, but less cost efficient!
Occasionally it is these cases with the relatives that makes you realise that is why you are a nurse. Because you can support these people in their time of need.
It is just as unfortunate though that you are a nurse, because you know what can happen to the human body. Sometimes I wish I knew nothing, just like Joe Public (before the internet that is!), then I would have not worry so much about what might kill me!!
The other day I had 4 cardiac arrests! 3 died and one I dispatched to the ward. 25% success, not bad for a failing trust. Cheating death is always a losing battle but I will give it my best shot. The only downside is the relatives. I have lost count of the times that I have had to tell a relative that their loved one has shuffled unwillingly off this mortal coil. It can be heartbreaking. I have not become immune to this suffering, it affects me, however I can often be strong to the point of brutal dispassion. I can often be weak as well.
The young drug addict who dies, the RTA who was drunk and crashed into a tree. These deaths although sad are emotionally reconcilable. The 32 year old cardiac arrest who just drops is just shit though. Most of the time in A&E and in the NHS it is just a case of processing patients. A bit like Tesco's, but less cost efficient!
Occasionally it is these cases with the relatives that makes you realise that is why you are a nurse. Because you can support these people in their time of need.
It is just as unfortunate though that you are a nurse, because you know what can happen to the human body. Sometimes I wish I knew nothing, just like Joe Public (before the internet that is!), then I would have not worry so much about what might kill me!!
All these blogs in one day....busy or what?
You may wonder why so much action has occured today on this blog spot. I have transferred entrys from a rival blog.com to blogger, and not wanting to let anyone miss out on the previous years blood sweat and beers (tears) I have proverbially 'cut and paste' to this site. They are all in correct order (unlike some of the cut and pastes our surgeons do at work), however that is another story.
Hung out to dry (or die) !!!
Had an 85 year old cardiac arrest. Had hung himself. Dead. He had tried two years ago with a shotgun. Obviously not successful. This time obviously he was.
Don't pee on my head and try and tell me its raining!
Doctors are funny beasts. We have a A&E SHO who appears to be obsessed with urine. Every patient, regardless of presenting complaint is required to produce a urine dip. It is getting extreme, the next cardiac arrest will undoubtably need one. Don't remember a UTI being a reversable cause of arrest. He becomes exceptionally agitated when water is not produced, as if it is our fault the demented lady in B bay can't give a sample, (not so much she can't pee as the bed will testify however getting it into a recepticle is another matter). The best trick is to use your nose. If they smell; UTI. Unless they come from a certain part of town, then its their natural aroma.
Ready Steady Cook...or not!!!!
Before starting in A&E, I nievely thought that vegetables, especially carrots were more sorted for eating, jullienne, diced or roughly chopped.
This young man, came in by ambulance (his first mistake) had allegedly been playing sex games with his girlfriend. (Miss July we think..well thats the edition of the mag he had). Anyway a carrot was now properly stuck up his bottom. Unable to get a clear X-Ray due to the translucency of the organic root veg it was left to our jovial Staff Grade to remove. Like a puppet master, the rather large hand of this doc dissapeared up this lads back passage. A quick root around and hey presto a 7" carrot appeared. A quick wash and it was returned to the lad for posterity. He then had to be admitted to ensure that he hadn't perforated his bowel. Lets just say that hospital dinners are shit at the best of times but we heard that the man was constantly asked if he wanted vegetables!! He probably got fed up by breakfast.
This young man, came in by ambulance (his first mistake) had allegedly been playing sex games with his girlfriend. (Miss July we think..well thats the edition of the mag he had). Anyway a carrot was now properly stuck up his bottom. Unable to get a clear X-Ray due to the translucency of the organic root veg it was left to our jovial Staff Grade to remove. Like a puppet master, the rather large hand of this doc dissapeared up this lads back passage. A quick root around and hey presto a 7" carrot appeared. A quick wash and it was returned to the lad for posterity. He then had to be admitted to ensure that he hadn't perforated his bowel. Lets just say that hospital dinners are shit at the best of times but we heard that the man was constantly asked if he wanted vegetables!! He probably got fed up by breakfast.
The Beginning
This is the start of an online journal of the ups and downs that becomes of a career within an Accident and Emergency department.
In order to adhere to the NMC Code of Conduct, names and my place of work have been changed or removed. However rest assurred, if you come to my department after doing something silly to your self you are fair game to my colleagues and myself. We have to have some entertainment.
In order to adhere to the NMC Code of Conduct, names and my place of work have been changed or removed. However rest assurred, if you come to my department after doing something silly to your self you are fair game to my colleagues and myself. We have to have some entertainment.
Subscribe to:
Posts (Atom)